Arthritis is a term that most people have heard, yet many misunderstand. It is not a single disease but rather a way to refer to joint pain or disease manifesting in more than a hundred different types. Each type has its symptoms and treatment methods, making it imperative for those suffering to understand what they are dealing with. Ignorance can lead to an escalation of symptoms or a delayed treatment plan, significantly impacting the quality of life. This article offers a detailed look at the most common types of arthritis and their associated symptoms. The goal is to help readers identify what might be plaguing them and what steps they should consider taking next.
Contents
Osteoarthritis (OA)
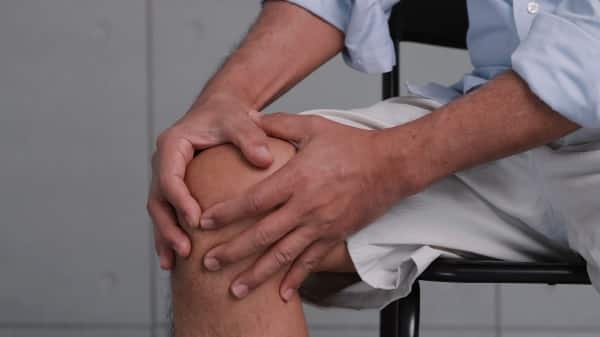
Osteoarthritis is one of the most prevalent forms of arthritis, affecting millions worldwide. It occurs when the cartilage at the end of the bones wears away due to age, obesity, injury, or overuse, leading to bones rubbing against each other. Osteoarthritis affects commonly used joints like knees, hips, hands, and spine. It’s often characterized by localized pain in these areas and stiffness, especially after inactivity or in the morning.
Unlike some other forms of arthritis that involve the immune system attacking the body’s tissues, osteoarthritis is primarily a degenerative condition. While there is no cure, treatments often include pain management, physical therapy, and, in severe cases, surgical intervention. Knowing the symptoms can help in early diagnosis and managing the condition better. Lifestyle changes, including regular exercise and weight loss, can significantly contribute to alleviating symptoms and improving quality of life.
Rheumatoid Arthritis (RA)

Rheumatoid arthritis differs from osteoarthritis in that it’s an autoimmune disease. The immune system mistakenly targets the synovium—the lining of the membranes surrounding the joints—resulting in inflammation that can eventually damage cartilage and bones. Commonly affected areas are smaller joints like those in the hands and feet. Due to its autoimmune nature, symptoms often extend beyond the joints and may include fever and fatigue.
The symptoms of rheumatoid arthritis can be particularly debilitating, affecting physical well-being and quality of life. It is often a chronic condition with flare-ups occurring periodically. Unlike osteoarthritis, which is more localized, rheumatoid arthritis usually affects joints on both sides of the body. Early diagnosis and aggressive treatment are crucial in managing the symptoms and preventing joint deformities. Treatment often involves medication to suppress the immune system, pain management, and sometimes surgery to repair damaged joints.
Psoriatic Arthritis
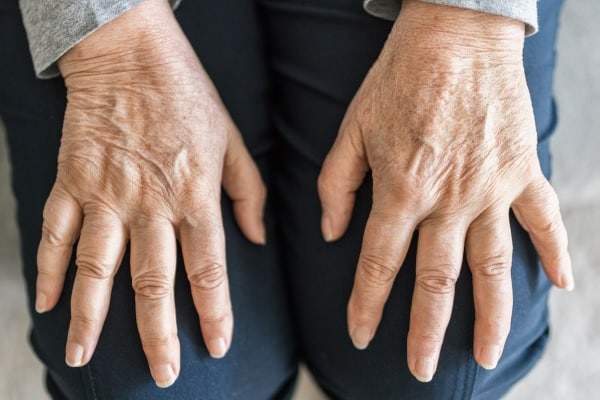
Psoriatic arthritis is an inflammatory form of arthritis that affects some people with psoriasis, a condition that causes red patches with silvery scales on the skin. Psoriatic arthritis often begins with skin symptoms before joint symptoms appear. The condition can affect any part of the body, including the fingertips and spine, and can range from mild to severe. The primary symptoms include joint pain, swelling, and stiffness, often accompanied by skin lesions.
Understanding the link between psoriasis and psoriatic arthritis is essential for effective treatment. While there’s no cure, the goal is to manage symptoms and prevent joint damage. Therapeutic options often involve medications that ease skin symptoms and relieve joint pain, such as biologics or disease-modifying antirheumatic drugs (DMARDs). Regular exercise, maintaining a healthy weight, and using joint protection techniques can also contribute to better management of the condition.
Gout
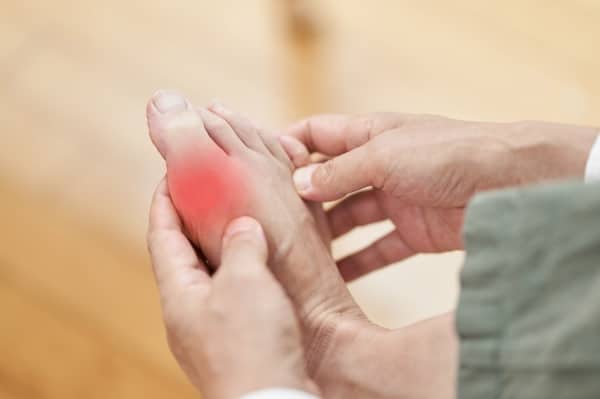
Gout is a form of arthritis often misunderstood as a lifestyle disease. It occurs due to the accumulation of urate crystals in the joints, leading to inflammation and intense pain. This build-up is often a result of high levels of uric acid in the blood, which can be influenced by diet, genetic factors, or the inability of the kidneys to filter out uric acid effectively. Gout usually affects the large joint of the big toe but can occur in other joints like the knees, elbows, and wrists.
The symptoms of gout are hard to ignore. They often come on suddenly and may include severe pain, redness, and swelling in the affected joint. Episodes, often called gout attacks, can last for days to weeks and may recur if the underlying issue of uric acid build-up is not addressed. Treatment focuses on relieving immediate symptoms through anti-inflammatory medications and long-term management, including dietary changes to lower uric acid levels. Gout is one form of arthritis where lifestyle changes can significantly impact the frequency and severity of episodes.
Ankylosing Spondylitis

Ankylosing spondylitis is a type of inflammatory arthritis that primarily affects the spine but can also involve other joints and even organs. Its hallmark feature is the fusion of the vertebrae, leading to a rigid and curved spine over time. The condition generally begins with lower back pain and stiffness and may gradually move upward along the spine. The pain often improves with exercise and worsens with rest, which sets it apart from other types of arthritis.
Management of ankylosing spondylitis requires a multidisciplinary approach involving medication, physical therapy, and sometimes surgical intervention. Treatments generally focus on controlling symptoms and preventing spinal deformity. Anti-inflammatory medications are commonly used to relieve pain and stiffness; in some cases, biologic medications are prescribed to slow the progression of the disease. Early diagnosis and treatment are crucial to minimize long-term complications and maintain a good quality of life.
Juvenile Arthritis

Juvenile arthritis is a term used to describe arthritis conditions that occur in children under 16. Contrary to popular belief, arthritis isn’t just an adult disease; it affects children, too. Juvenile arthritis usually manifests as persistent joint pain, swelling, and stiffness, similar to adult forms. However, because it occurs at a developmental stage, it can have a more pronounced impact on a child’s growth and development.
Unlike adult arthritis, which is often lifelong, many children with juvenile arthritis outgrow the condition as they reach adulthood. However, early and aggressive treatment is essential to control symptoms and minimize long-term joint damage. Treatment usually involves a combination of medication, physical therapy, and lifestyle adjustments. Parents and caregivers play an integral role in managing juvenile arthritis, from ensuring medication adherence to helping the child maintain an active lifestyle.
Lupus

Lupus is an autoimmune disease that shares some similarities with arthritis, primarily in how it can affect the joints. While it’s not a type of arthritis, many people with lupus experience arthritis-like symptoms, including joint pain, stiffness, and swelling. The disease is often systemic, affecting other organs like the kidneys, skin, and lungs.
Diagnosing lupus can be complicated due to its wide range of symptoms. Because it mimics several other conditions, including arthritis, a thorough medical evaluation is necessary for diagnosis. Treatment generally focuses on managing symptoms and may include antimalarial drugs, corticosteroids, and immune-suppressing drugs. Like other autoimmune conditions, early diagnosis and treatment are critical in managing symptoms and preventing organ damage.
The Bottom Line
Arthritis is a complex set of conditions with multiple types and many symptoms. Understanding the specifics of each type is critical for proper diagnosis and effective treatment. Each type has unique challenges and symptomatology, and what works for one may not work for another. The best action is to consult a healthcare professional for an accurate diagnosis and tailored treatment plan. Managing arthritis may be challenging, but it’s far from impossible. With proper care, most people with arthritis can lead fulfilling lives, with their symptoms well-managed and their daily activities largely unhindered.



the food chains have plenty blame on this matter , and also the way one sleeps also , bad chemicals and sugars and GOD only knows what they put in the foods and the drinks